INTERGROWTH-21st
Activities in different countries
Text prepared by Sandy Savini
Goals and Objectives
The INTERGROWTH-21st Project has five objectives. The first three are to produce, for practical clinical applications and to monitor population trends, sets of international growth standards describing:
- Fetal growth from early pregnancy (Fetal Growth Longitudinal Study—FGLS).
- Postnatal growth of preterm infants (Preterm Postnatal Follow-up Study—PPFS).
- Birthweight, length and head circumference for gestational age (Newborn Cross-sectional Study—NCSS).
These standards will be related to perinatal morbidity and mortality to identify levels of risk.
The remaining two objectives are:
- To investigate the determinants of preterm delivery and impaired fetal growth in this sample (Preterm and Impaired Fetal Growth Syndromes Study—PIF-GSS).
- To develop a prediction model, based on multiple two-dimensional (2D) ultrasound measurements, for estimating gestational age during mid–late pregnancy for use in women without access to early/frequent antenatal care (Mid-late Pregnancy Gestational Age Prediction Study—MPGAPS).
Project Design and Implementation
Three population-based studies were implemented at each study site:
- Fetal Growth Longitudinal Study (FGLS) from <14 +0 weeks gestational age to birth to monitor and measure fetal growth clinically (Symphyseal-fundal-height) and by ultrasound in a healthy population.
- Preterm Postnatal Follow-up Study (PPFS) of preterm infants (>26 +0 but <37 +0 weeks) in the FGLS to describe their postnatal growth pattern.
- Newborn Cross-sectional Study (NCSS) of all newborns at the study centres over 12 months, obtaining anthropometric measurement and neonatal morbidity and mortality rates.
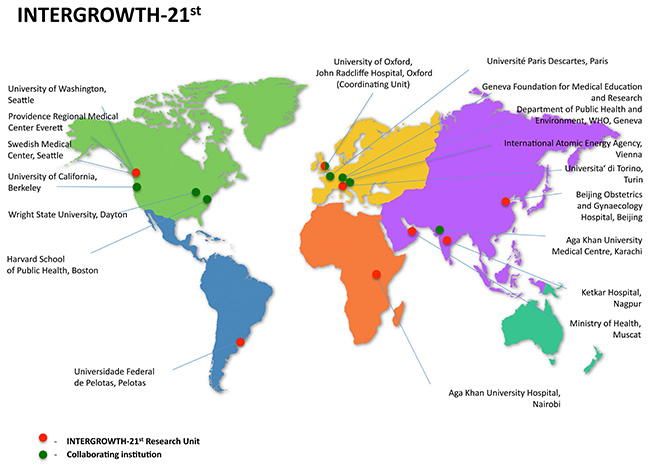
The recruitment for the study took place between April, 2009 and March, 2014 in eight study sites: the cities of Pelotas (Brazil), Turin (Italy), Muscat (Oman), Oxford (UK), Seattle (USA); Shunyi County, Beijing (China), the central area of Nagpur (India) and the Parklands suburb of Nairobi (Kenya). Each site contributed a population-based sample of healthy pregnant women expected to provide full growth potential to their foetuses, making it possible to produce prescriptive standards similar to the WHO Child Growth Standards.
The study populations obtained from these geographically defined areas (e.g. city or county) had no socio-economic constraints on growth, low morbidity and perinatal mortality and adequate nutritional status. To be included, women were non-smokers, with a normal pregnancy history, and without health problems likely to influence fetal growth or indicate a risk for pregnancy-related pathological conditions.
- In FGLS, women were screened before 14 +0 weeks at the time of their first antenatal visit and followed-up with standard clinical and 2D ultrasound examinations every five weeks, i.e. up to six times during pregnancy.
- In PPFS, preterm infants (>26 +0 but <37 +0 weeks) born from this sample were followed-up during the first 8 months of life with the same protocol and set of anthropometric measures that were used in the WHO Child Growth Study. Postnatal growth was evaluated from both delivery and conception for comparison with the corresponding in utero measurements.
- In the NCSS study, all newborns at the study centres, born during a fixed (e.g. 12 month) period, had anthropometric measurements taken immediately after birth. Only babies born to women who met the same inclusion criteria used in FGLS were selected to construct the newborn standards. Birth weight and gestational age was also related to neonatal morbidity and mortality outcomes to construct risk-related newborn weight for gestational age standards.
Exactly 4,607 pregnancies were included in FGLS allowing for 193 preterm infants to be included in PPFS. In NCSS, 60,268 newborns were recruited, of whom 20,486 were eligible for the standards.
Standardisation and Quality Control
Standard quality control measures were employed using a random evaluation of ultrasound measurements (from stored images) to monitor validity and reliability. A team of experienced obstetric ultrasonographers and neonatal anthropometrists were trained and formed the research teams at each study site, and anthropometric measures were monitored and standardised centrally. All data were entered and managed in an on-line data management system specifically developed for the study, including a system for direct transfer of blinded data from the ultrasound equipment to the database. This on-line system allowed a continuous assessment of all data collected and the initiation of data management and analysis soon after data collection was completed. Data from all sites were pooled to construct the international fetal, newborn and preterm growth standards following the same analytical strategy that was used to develop the WHO Child Growth Standards.
Global Perinatal Package
The INTERGROWTH-21st Project has led the way to producing a Global Perinatal Package. These resources will be released from August 2014 onwards. Resources on how to use the Global Perinatal Package will be available in the Training Toolkit. Please continue to check this website for the latest updates. Included in the Package will be the following:
Optimizing Public Health Outcomes
These new fetal and newborn standards, when incorporated into health services, will be unique tools for evidence-based estimation of under-nutrition at birth, maternal and perinatal programme monitoring and the clinical care of newborns worldwide, specifically in developing countries where most of these health problems exist. When fully implemented, the growth charts they have developed should benefit all pregnancies throughout the world because fetal growth is currently evaluated using clearly limited tools, and this should also provide major clinical and economic benefits. The preterm and newborn charts will be of greatest benefit in developing countries where most morbidity and mortality amongst newborns (especially growth restricted and preterm babies) occur.
The Standard Operating Procedures (SOPs) and study protocols used to implement the INTERGROWTH-21st Project are available here. Please visit the INTERGROWTH-21st Project study website for further detailed information about the study.
